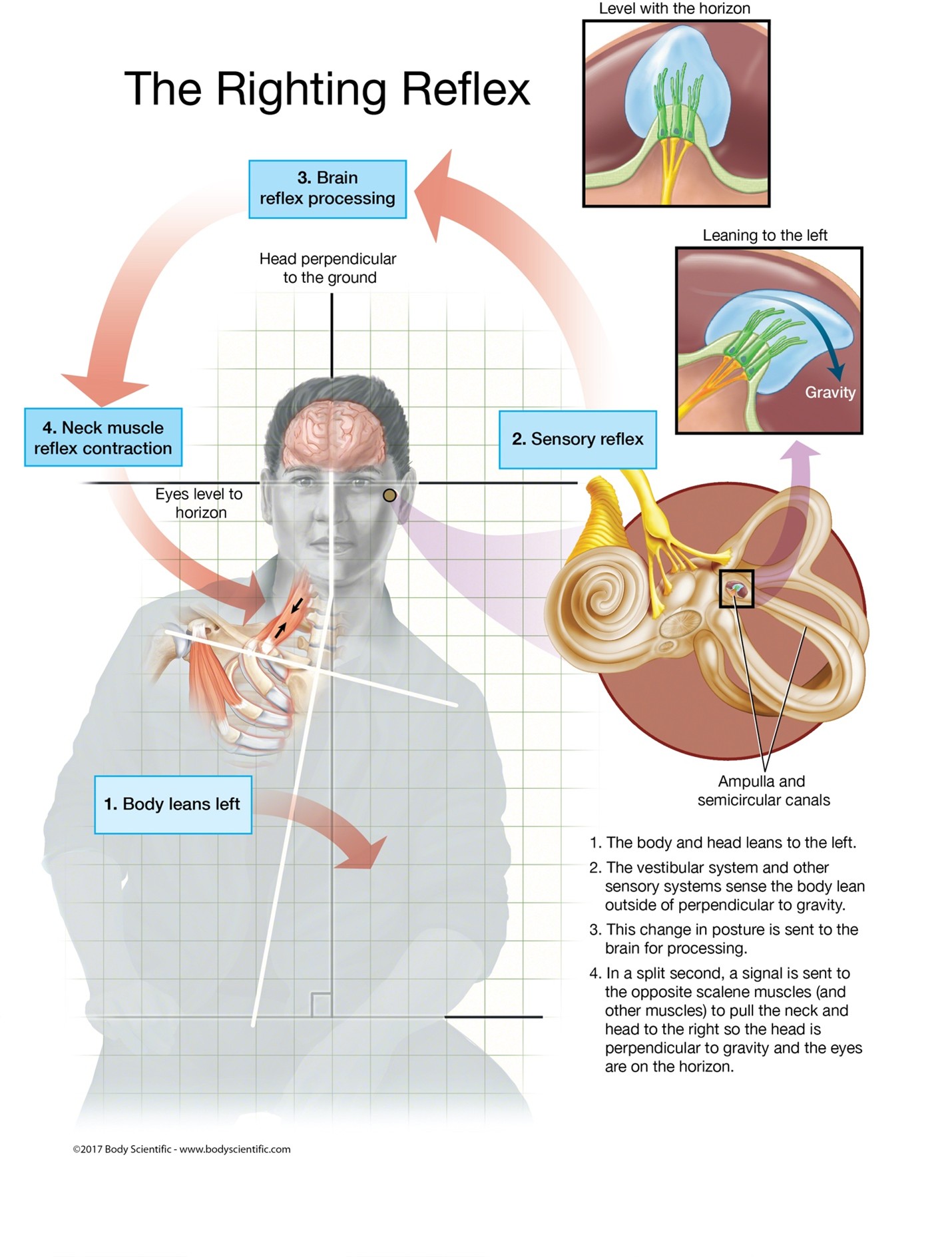
When the body leans to one side, the head naturally shifts the opposite way to stay level. This balancing action happens through automatic reflexes that keep your eyes and inner ear aligned with the horizon. In my clinical experience, many individuals do not realize how much work the neck muscles perform during these simple postures. When the head weighs nine to twelve pounds, even a small tilt can load the muscles surrounding the upper ribs and neck.
A common area involved in this balancing reflex is the scalene muscle tension pattern. These muscles stabilize the neck when the head moves or when the torso leans. Many individuals describe feeling pulling sensations in the lower neck when they rest into one side for long periods. This becomes more noticeable when the head tilts for reading or looking at a device.
When the torso shifts left, the head shifts right. This triggers what is known as the righting reflex, a neurological response that keeps the eyes level. The body relies on this reflex to avoid dizziness or imbalance. As the head tilts, the scalenes on one side tighten to support the weight. Over time, this may increase brachial plexus pressure, especially when the surrounding muscles remain active for extended periods.
Patients often report feelings that resemble shoulder girdle tightness or a sense of heaviness along the arm. These sensations can come from the way prolonged leaning loads the neck muscles. Even simple posture can influence the spaces where nerves and vessels pass between the clavicle and first rib. In my clinical experience, this is a pattern I commonly see in office workers and individuals who lean toward one side of a chair.
Long-positioned leaning can create chronic neck muscle overload. This may lead to irritation in tissues that support the collarbone and upper ribs. Many individuals describe this as a deep, dull feeling that slowly develops during the day. When the scalenes engage continuously, they may contribute to thoracic outlet compression symptoms, especially when other surrounding tissues become irritated.
The body responds to irritated tissues through protective guarding. When nerves detect inflammation, they send signals to the brain indicating that something needs protection. The brain responds with an automatic tightening known as protective muscle splinting. This splinting can make the neck feel stiff when turning or looking down.
Over time, this splinting may contribute to upper rib elevation, a pattern that reduces mobility in the spaces under the collarbone. Patients often report that their chest or shoulder feels lifted on one side. When tension remains long-term, individuals may experience what they describe as arm fatigue with posture, especially while typing or holding a device.
The cycle continues when inflammation persists. As tissues become irritated, the reflexive tightening becomes more pronounced. Many individuals describe this cycle as tension that won’t release, even after stretching or resting. These patterns are often related to positions rather than one specific movement.
The simple act of stacking the head over the torso can help reduce unnecessary muscle activation. Keeping the ears aligned over the shoulders allows the neck muscles to remain balanced. This can reduce the need for the righting reflex to overwork. Many individuals find that postural awareness for TOS, practiced throughout the day, helps them understand how often they lean unconsciously.
Some people explore gentle tools to help with relaxation. The Vibeassage®, Vibeassage® Sport, Vibeassage® Pro, and TDX3 soft-as-the-hand Biomimetic Applicator Pad are often mentioned in educational discussions about how people perceive tissue vibration. In my clinical experience, many individuals describe that vibration for neck relaxation, when understood properly, helps them become more aware of areas that feel tense.
Understanding posture can help individuals interpret sensations related to nerve sensitivity around the collarbone. For some, leaning positions lead to increased awareness of changes in circulation. They sometimes describe arm tingling with head tilt, especially during long hours at a desk. These patterns often change when posture changes.
When the upper ribs stiffen, individuals may experience reduced first rib mobility. This can influence shoulder mechanics and how the clavicle moves. Many describe this as a catching sensation during daily activities. Leaning can intensify these sensations.
Daily leaning often affects cervical posture mechanics. When the head stays off-center, neck joints may experience uneven pressure. This may contribute to stiffness with rotation, especially when looking over one shoulder repeatedly.
Some individuals experience upper chest tightness in response to prolonged leaning. This may affect how the shoulder blade glides. The body adapts through patterns of guarding that can influence nerve glide restrictions along the arm.
Prolonged leaning also influences seated posture habits. These habits can lead to compensations in breathing mechanics. Many individuals notice shallow breathing with tension when their posture collapses.
The interplay between posture, reflexes, and muscle tension can change the space where nerves and blood vessels travel. This may create collarbone area pressure, especially during repetitive tasks. Individuals sometimes describe this as a fullness or warm sensation.
As leaning continues, patterns of upper trapezius guarding may appear. This adds to the overall sensation of tension. Combined with scalene activation, it may contribute to neck and shoulder imbalance.
Individuals who repeat these positions often report tightness near the first rib, especially after long static tasks. This is often described as a deep area of discomfort. Awareness practices that improve ergonomic head alignment can help reduce unnecessary muscle loading.
These tension patterns may also influence nerve-related shoulder sensations. Many individuals report that these sensations become more noticeable when posture worsens throughout the day.
Understanding these patterns can help individuals recognize early TOS-related warning signs. They may also notice repetitive leaning triggers, which often contribute to symptom flares.
Over time, the cycle of leaning, tension, guarding, and reflexive holding may contribute to chronic postural strain throughout the neck and upper chest. By stacking the head over the torso and allowing the body to relax, individuals can let reflexes recalibrate naturally. This simple awareness practice helps them understand how posture influences tension patterns during daily life.
Team Doctors Resources
✓ Check out the Team Doctors Recovery Tools
The Vibeassage Sport and the Vibeassage Pro featuring the TDX3 soft-as-the-hand Biomimetic Applicator Pad
https://www.teamdoctors.com
✓ Get Dr. Stoxen’s #1 International Bestselling Books
Learn how to understand, examine, and reverse your TOS—without surgery.
https://drstoxen.com/1-international-best-selling-author
✓ Check out Team Doctors Online Courses
Step-by-step video lessons, demonstrations, and self-treatment strategies.
https://teamdoctorsacademy.com
✓ Schedule a Free Phone Consultation With Dr. Stoxen
Speak directly with him so he can review your case and guide you on your next steps.
https://drstoxen.com/appointment
#thoracicoutletsyndrome #TOS #neckpain #scalenes #brachialplexus #first rib #posture #nervecompression #vascularcompression #upperbodytension #deskposture #ergonomics #shoulderpain #armtingling #neckstrain #posturalhabits #inflammation #muscleretention #mobilitytips #TeamDoctors
References
- Hooper, T. L., Denton, J., McGalliard, M. K., Brismee, J. M., & Sizer, P. S. “Thoracic Outlet Syndrome: A Controversial Clinical Condition.” Part 1: Anatomy, Diagnosis, and Classification. Journal of Manual & Manipulative Therapy. https://doi.org/10.1179/2042618613Y.0000000024
- Povlsen, B., Hansson, T., & Povlsen, S. D. “Diagnosing Thoracic Outlet Syndrome: Current Approaches and Future Directions.” https://doi.org/10.3390/diagnostics8010003
- Illig, K. A., et al. “Reporting Standards of the Society for Vascular Surgery for Thoracic Outlet Syndrome.” Journal of Vascular Surgery. https://doi.org/10.1016/j.jvs.2016.01.040
- Likes, K., Rochlin, D. H., Call, D., & Freischlag, J. A. “Neurogenic Thoracic Outlet Syndrome: Patient Characteristics and Diagnosis.” Annals of Vascular Surgery. https://doi.org/10.1016/j.avsg.2013.04.016

Dr James Stoxen DC., FSSEMM (hon) He is the president of Team Doctors®, Treatment and Training Center Chicago, one of the most recognized treatment centers in the world.
Dr Stoxen is a #1 International Bestselling Author of the book, The Human Spring Approach to Thoracic Outlet Syndrome. He has lectured at more than 20 medical conferences on his Human Spring Approach to Thoracic Outlet Syndrome and asked to publish his research on this approach to treating thoracic outlet syndrome in over 30 peer review medical journals.
He has been asked to submit his other research on the human spring approach to treatment, training and prevention in over 150 peer review medical journals. He serves as the Editor-in-Chief, Journal of Orthopedic Science and Research, Executive Editor or the Journal of Trauma and Acute Care, Chief Editor, Advances in Orthopedics and Sports Medicine Journal and editorial board for over 35 peer review medical journals.
He is a much sought-after speaker. He has given over 1000 live presentations and lectured at over 70 medical conferences to over 50,000 doctors in more than 20 countries. He has been invited to speak at over 300 medical conferences which includes invitations as the keynote speaker at over 50 medical conferences.
After his groundbreaking lecture on the Integrated Spring-Mass Model at the World Congress of Sports and Exercise Medicine he was presented with an Honorary Fellowship Award by a member of the royal family, the Sultan of Pahang, for his distinguished research and contributions to the advancement of Sports and Exercise Medicine on an International level. He was inducted into the National Fitness Hall of Fame in 2008 and the Personal Trainers Hall of Fame in 2012.
Dr Stoxen has a big reputation in the entertainment industry working as a doctor for over 150 tours of elite entertainers, caring for over 1000 top celebrity entertainers and their handlers. Anthony Field or the popular children’s entertainment group, The Wiggles, wrote a book, How I Got My Wiggle Back detailing his struggles with chronic pain and clinical depression he struggled with for years. Dr Stoxen is proud to be able to assist him.
Full Bio) Dr Stoxen can be reached directly at teamdoctors@aol.com